 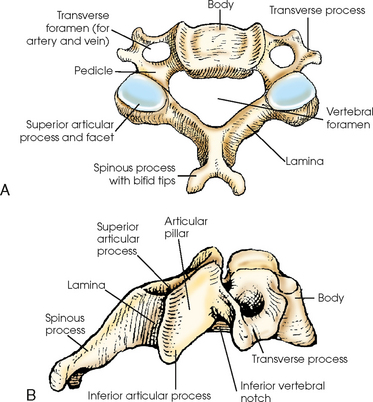
Osteoarthritis is often viewed as a disease of articular cartilage loss and bony proliferation however, the process of failure involves the whole joint complex, which includes the cartilage, subchondral bone, synovium, joint capsule, ligaments, and periarticular paraspinal muscles and associated soft tissues. In humans, vertebral osteoarthritis is a clinical and pathological disorder that involves both structural and functional failure of the synovial articulations. Therefore, little is known about the etiopathogenesis and clinical effects of osteoarthritis within the equine cervical vertebrae. A further complication is that radiographic and histologic evidence of osteoarthritis is prevalent in horses with and without clinical signs of neck pain or stiffness. 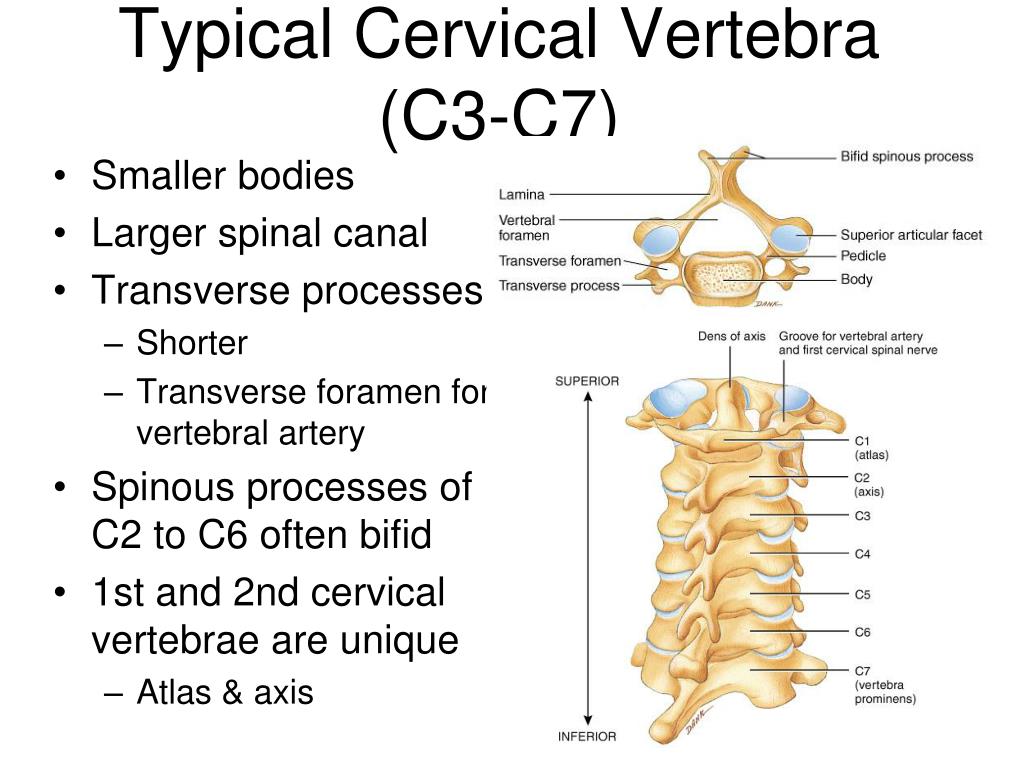
The clinical effects of cervical osteoarthritis in the absence of cervical myelopathy are not commonly reported or considered. Concurrent osteophyte production has also been reported in studies on cervical vertebral instability however, enlarged or encroaching articular processes associated with osteoarthritis are often considered a secondary contributing factor to spinal cord compression rather than as a primary disease process. Review of the equine literature suggests that cervical vertebral myelopathy is one of the primary disease processes affecting the equine cervical region. Neck pain and stiffness are becoming more commonly recognized clinical entities in horses due to increased awareness of potential adverse effects on athletic performance, use of detailed spinal evaluation procedures (e.g., acupuncture, chiropractic), and improved diagnostic imaging (e.g., ultrasonography, computed tomography) of this body region. The clinical significance of the described lesions is unknown, but the findings are expected to enhance the reporting of articular process and periarticular changes noted on advanced diagnostic imaging of the equine cervical and cranial thoracic vertebral regions. A high prevalence and wide variety of abnormal bony changes of varying severity were found in articular processes across all vertebral levels. The grade of osseous pathology was positively associated with both age and wither height. Most paired articular surfaces and left-right grades of severity were not significantly different. The highest prevalence of mild changes was localized to the C3-C6 vertebral levels moderate changes to C6-T2 and severe changes to C2-C3 and C6-T2. Overall grades of severity included: normal (28%), mild (45%), moderate (22%), and severe (5%). Osteophyte formation was the most common bony change noted. Seventy-two percent of articular processes had bony changes that were considered abnormal. Data were analyzed to compare alterations in joint margin quadrants, paired articular surfaces within a synovial articulation, left-right laterality, and vertebral level distributions and to determine associations with age, wither height and sex. Cranial and caudal articular processes of the cervical and first three thoracic vertebrae (C2-T3) from 55 horses without a primary complaint of neck pain were evaluated for the presence and severity of abnormal bony changes. The objectives of this observational, cross-sectional study were to characterize and establish the prevalence of osseous proliferation of articular surfaces, joint margins and adjacent soft tissue attachments (i.e., joint capsule and deep spinal muscles) in a mixed population of horses of variable ages, sizes, and breeds to better capture the full spectrum of disease affecting the cervical articular processes. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
